
image credit The Johns Hopkins Bloomberg School of Publich Health
SUMMARY
In August 2022, the U.S. Food and Drug Administration (FDA) authorized bivalent COVID-19 vaccine formulations as single booster doses. These bivalent formulations contain messenger RNA (mRNA) from the original SARS-CoV-2 strain and mRNA present in the BA.4 and BA.5 lineages of the Omicron variant. Contrary to some viral claims online that these boosters weren’t adequately tested, the FDA based its decision to authorize these vaccines on clinical evidence of the safety and efficacy of previous vaccines with similar composition and technology.
Introduction
On 31 August 2022, the U.S. FDA announced in a press release that it had authorized two bivalent COVID-19 vaccine formulations for use as a single booster dose following primary COVID-19 vaccination. These were the Moderna COVID-19 bivalent vaccine for use in adults, and the Pfizer-BioNTech COVID-19 bivalent vaccine for use in individuals 12 years of age and older.
A bivalent vaccine produces an immune response against two different antigens. This can mean two different viruses, or in the case of bivalent COVID-19 vaccines, two variants of the same virus. Examples of multivalent vaccines include the quadrivalent influenza vaccine, which protects against two influenza A and two influenza B viruses, and the Gardasil-9 vaccine, which targets nine strains of human papillomavirus (HPV).
The original formulations of the COVID-19 vaccines target the spike protein of the initial SARS-CoV-2 strain. One of the key motivations for developing bivalent COVID-19 vaccines is our knowledge that differences in the spike protein can change the virus’ ability to cause disease and evade the immune system. Such changes have significant implications for the level of protection provided by the original vaccines.
The core aim of the bivalent vaccine booster remains identical to that of the original COVID-19 mRNA vaccines: to induce an immune response against the spike protein of SARS-CoV-2 that will protect against disease. The difference is that the bivalent vaccines will be able to induce immunity specific to the mutated spike protein in variants.
Bivalent vaccines aim to target the dominant Omicron variants
The authorized COVID-19 bivalent vaccines contain mRNA molecules that encode for the spike protein of the original SARS-CoV-2 strain and the spike protein of the Omicron BA.4 and BA.5 variants. The spike protein is identical in the BA.4 and BA.5 variants, but distinct from the original strain.
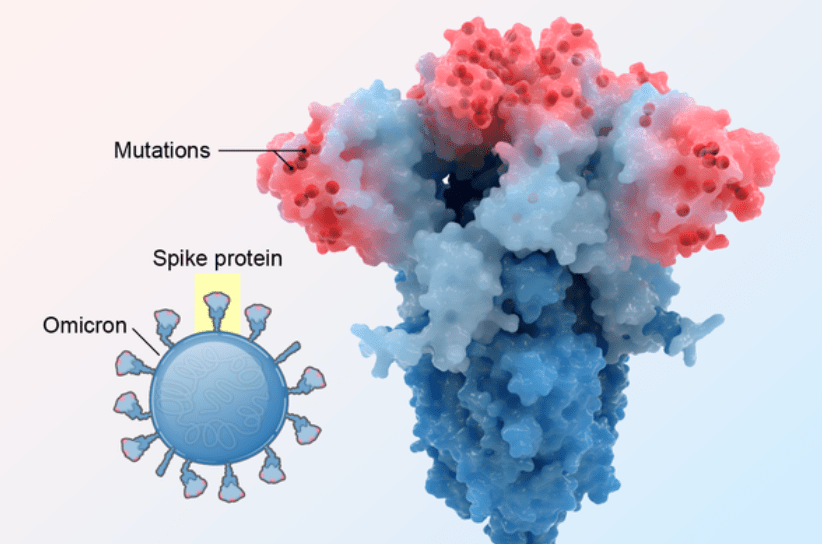
Figure 1. Antibodies bind to specific regions of the spike protein to neutralize SARS-CoV-2. Mutations in the receptor-binding domain of the spike protein in the Omicron variant make it difficult for antibodies that are effective against other variants to bind and neutralize the virus. Source: Scientific American.
The bivalent COVID-19 vaccines have been designed to provide better protection against COVID-19 caused by the Omicron variant than the original formulation targeted against the initial strain of the virus. There has been some discussion among scientists whether a monovalent booster tailored for BA.4 and BA.5 would have achieved the same objective more efficiently than a bivalent booster for both the original strain, BA.4 and BA.5.
The BA.4 and BA.5 lineages became predominant in the U.S. in June 2022, accounting for more than half of the COVID-19 cases in the country at that time, as reported by Reuters. At the time of writing, both lineages continue to account for more than half of COVID-19 cases in the U.S., according to data collected by the U.S. Centers for Disease Control and Prevention (CDC).
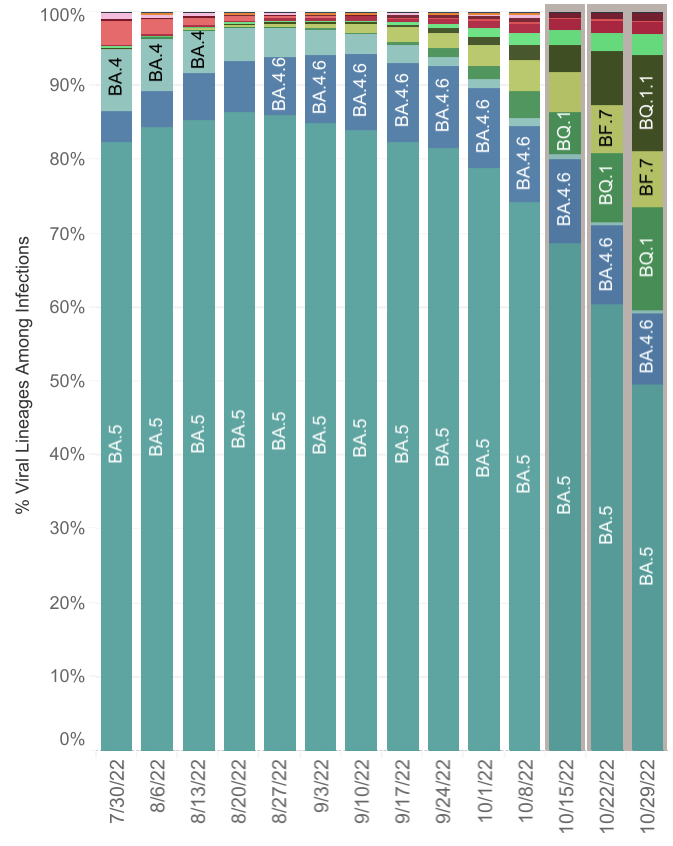
Figure 2. Proportion of SARS-CoV-2 variants among total infections in the U.S. Weekly data between 30 July 2022 and 29 October 2022. Data between 15 October 2022 and 29 October 2022 include Nowcast projections, a model that allows for more recent estimates of the circulating variants. Source: CDC.
Authorization is based on existing evidence from clinical trials in people
The recently authorized boosters aren’t the first bivalent COVID-19 vaccines. Earlier bivalent formulations, specifically the Pfizer-BioNTech and Moderna vaccines targeting the original strain and the BA.1 variant, were tested for safety and efficacy in clinical trials that included several hundreds of adults.
The FDA based its authorization on safety and effectiveness data for the original COVID-19 vaccines. In addition, it also reviewed the induced immune response and safety data from clinical studies of bivalent COVID-19 vaccines targeting the BA.1 variant, considered to be similar to the new formulations.
Although the results of the clinical trials of the bivalent BA.1 vaccines haven’t yet been published, the results were described in press releases by Pfizer and BioNTech as well as by Moderna. At the 30 and 60-microgram doses, the Pfizer-BioNTech vaccine showed a nine to 11-fold increase in viral neutralization response against the BA.1 variant compared to the company’s original vaccine. The Moderna vaccine showed that the viral neutralization response against Omicron was approximately eight-fold higher than the company’s original vaccine.
Both companies reported that the bivalent vaccines demonstrated a favorable safety and tolerability profile, similar to that of the original vaccines. The most commonly reported side effects among participants of trials of bivalent vaccines, according to the FDA news release, included pain, redness and swelling at the injection site, muscle pain, joint pain, chills, fever, fatigue, headache, and nausea/vomiting.
The European Medicines Agency (EMA) also endorsed the bivalent COVID-19 vaccines, approving the Moderna and Pfizer-BioNTech bivalent vaccines for the original strain of SARS-CoV-2 and the BA.1 variant, as well as the Pfizer-BioNTech bivalent vaccines for the original strain of SARS-CoV-2 and the BA.4 and BA.5 variants.
The EMA based its endorsement of bivalent COVID-19 vaccines on existing clinical data, noting that bivalent vaccines for the BA.1, BA.4, and BA.5 lineages have the same composition, as well as “similar safety profiles and predictable immune responses against the strains they target”.
In addition to the existing clinical data, the U.S. FDA also based its authorization of the Pfizer-BioNTech bivalent vaccine on some nonclinical data in mice. The researchers evaluated the immune response to the bivalent COVID-19 vaccine targeting the original strain and the BA.4 and BA.5 lineages in a group of eight mice.
The group of mice that received the bivalent vaccine (original strain + BA.4 and BA.5) had a viral neutralization response that was 2.6 times higher against Omicron BA.4 and BA.5 than those that received the original vaccine formulation and a 4.8-fold better viral neutralization response than those that received the monovalent vaccine modified for Omicron BA.1.
Vaccines are designed to be regularly updated without new clinical trials
The decision to authorize bivalent vaccines for the BA.4 and BA.5 variants without testing them in clinical trials has become fodder for vaccine misinformation, as can be seen in this Instagram reel casting doubts on the safety of vaccine boosters. However, not testing updated vaccines in clinical trials is normal. In fact, this is the case for influenza vaccines, which are updated every year to target current strains of the flu virus without having to undergo clinical trials.
Similarly, the bivalent vaccines for the BA.4 and BA.5 variants use the exact same technology and contain the same ingredients than the already-authorized or approved COVID-19 vaccines. Since the vaccine composition is the same, there’s no plausible reason to believe the safety profile of the bivalent boosters will change. In other words the safety of the updated vaccines is supported by earlier clinical trials of the original formulation.
This approach allows researchers to tailor vaccines and respond to the dominant variants of a virus in a timely fashion, as Claude-Agnès Reynaud, the director of research at France’s Necker-Enfants Malades Institute, told AFP:
“The goal of mRNA vaccines is to be able to adapt to the variants of the virus. By doing a clinical trial, we would have the result in six months. By then, another variant may be there.”
A clinical trial for the Pfizer-BioNTech bivalent BA.4 and BA.5 vaccine started in September 2022. In a press release in mid-October 2022, Albert Bourla, the chairman and CEO of Pfizer, explained that this trial is in line with the company’s policy of transparency regarding COVID-19 vaccines.
The press release reported “positive” early data from this trial, which showed that the bivalent vaccine was well tolerated, with a safety profile similar to that of the original COVID-19 vaccine. The data also suggested that the bivalent vaccine provides better protection against the BA.4 and BA.5 variants than the original vaccine.
In conclusion, previous clinical trials of the original COVID-19 vaccines and earlier bivalent vaccine formulations provide us with sufficient clinical evidence for the safety of the recently authorized bivalent boosters. These vaccines have an almost-identical composition as the bivalent vaccines for the BA.1 variant, differing only in the mRNA sequence encoding the spike protein. Certain social media posts claiming that the bivalent vaccines were inadequately tested are misleading, because both the FDA and the EMA based their decision to authorize these vaccines on the clinical evidence of safety and effectiveness of previous COVID-19 vaccines of the same composition and technology.
