- Health
Potential role for T cells in COVID-19 immunity accurately reported in National Geographic article
Reviewed content
Headline: "Why antibodies may not be the key to beating coronavirus"
Published in National Geographic, by Carrie Arnold, on 2020-08-07.

Review
An article published in National Geographic summarizes the recent findings of several research groups suggesting that T cells may play a role in the body’s immune response against the virus SARS-CoV-2 and discusses the implications of T cell involvement. According to social media research tool Buzzsumo, the article has received more than 13,000 interactions, including likes, shares, and comments, on Facebook.
Scientists who reviewed the article found that it accurately reported the current body of knowledge regarding T cell contribution to immunity against SARS-CoV-2. They agreed that these findings are intriguing and highlight the important role that T cells play in antiviral immune responses in general. “The immune response is a complex subject which is very difficult to describe in a lay manner, however the author effectively utilized military metaphors to explain the basics of B and T cells in fighting disease,” said Leigh Jones, Head of Training at Oxford University’s Clinical Research Unit. More importantly, she found that the key findings of recent studies regarding cross-reactive memory T cells[1,2]) were communicated truthfully with the aid of scientists who had worked on those studies. [See our reviewers’ overall feedback.]
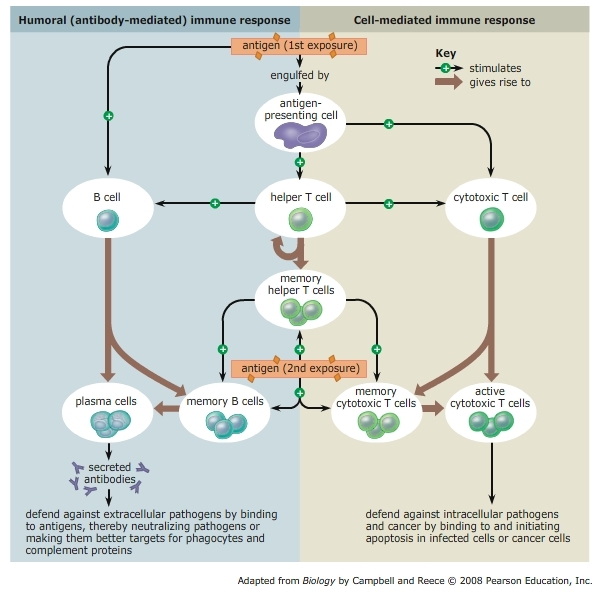
T cells and B cells comprise a part of the immune system termed the adaptive immune system (Figure 1). B cells produce antibodies, whereas T cells contribute to immune defenses in different ways. Some types of T cells directly kill infected cells, while others coordinate and regulate the immune response through chemical interactions with other immune cell types[3].
Antibody testing and studies related to COVID-19 have frequently made news headlines, but relatively less attention has been paid to T cells even though they play an important role in clearing viral infections. A key reason for this, as the article correctly points out, is that antibody levels are much easier and quicker to measure in the laboratory, whereas it is technically difficult and time-consuming to measure T cell responses. Hence T cell studies are scarce and their relevance to the immune response against SARS-CoV-2 was initially overlooked, leading Eric Topol, a cardiologist and professor of molecular medicine at the Scripps Research Institute, to advise in the following Twitter thread that “when you interpret seroprevalence, serology, antibody only data, please keep [in mind] the incomplete nature of that assessment in terms of the broader cellular immune response to [SARS-CoV-2]. There’s a lot more to learn about the stuff we don’t measure.”
When we don't measure important stuff.
A thread about the immune response to #SARSCoV2
1. Since serology/IgG can be readily measured, this is what is conventionally used to assess an individual's response
That's a very incomplete picturehttps://t.co/T49ckLHBNr pic.twitter.com/IKSlrrGpXh— Eric Topol (@EricTopol) July 1, 2020
But that has changed in recent months, with results from a few studies shedding light on the potential involvement of T cells in COVID-19 immunity. Specifically, the National Geographic article delves into studies by researchers at the Karolinska Institute in Sweden, the La Jolla Institute of Immunology in the United States, and Duke-NUS Medical School in Singapore, which we describe briefly below.
Sekine et al. published a study in Cell which reported the presence of SARS-CoV-2-specific memory T cells in COVID-19 patients[4]. This type of T cell is important for protecting against future reinfection, as it enables the immune system to recognize a pathogen that it has encountered in the past. They also found that this type of T cell was also present in some people who had no detectable antibodies against two types of SARS-CoV-2 proteins, more specifically the nucleocapsid (N) and spike (S) proteins. This finding suggests that antibody levels alone may not provide us with the complete picture of the immune response against COVID-19, and that it may also be important to measure T cell responses during vaccine trials.
A study by Grifoni et al. published in the journal Cell found that T cells in 40%–60% of individuals who had not been exposed to SARS-CoV-2 were still able to recognize different proteins on SARS-CoV-2[1]. Later, a study by Mateus et al., published in Science and led by many of the scientists who co-authored the Cell study, discovered that these T cells found in unexposed individuals were memory T cells that arose from prior infection with other coronaviruses that cause the common cold[2]. These findings were corroborated by a study from Le Bert et al. who reported that SARS-CoV-1 patients, who were infected 17 years ago, possessed memory T cells that are capable of recognizing the N protein on SARS-CoV-2[5]. The ability of these memory T cells to recognize proteins on SARS-CoV-2 is very likely due to similarities between these proteins among members of the coronavirus family.
Altogether, the findings of these studies suggest that a prior history of infection with other coronaviruses may prime the immune system to recognize SARS-CoV-2 through persistent, cross-reactive memory T cells. In theory, these T cells could mediate an immune response against SARS-CoV-2. Hanif Javanmard Khameneh, a postdoctoral researcher at the Institute for Research in Biomedicine at the University of Lugano in Switzerland, said that these findings provide “a very interesting concept which has to be studied more in detail to establish its relevance.”
These results also show that scientists need to take into account the role of memory T cells in COVID-19 vaccine development, as highlighted in a comment by Angéline Rouers, a research fellow at the Singapore Immunology Network (see below). The levels of memory T cells in the body may be an important correlate of protection (an indicator showing that a vaccine confers protection against the disease) like antibody titers[6], especially since some studies have raised concerns about waning antibody levels over time[7,8]. A vaccine candidate’s ability to stimulate the formation of memory T cells may therefore provide scientists with a better indicator of long-term protection.
It is important to keep in mind that these findings do not mean that antibodies are not needed or important for mounting a successful immune response against viruses like SARS-CoV-2. In fact, the National Geographic article correctly points out that antibodies contribute to protection by binding to the virus and preventing it from entering and infecting cells.
Another important caveat of these T cell studies is that they have not established that the presence of cross-reactive memory T cells is associated with protection against COVID-19 or with less severe disease in people. While they offer clues that provide a foundation for further studies, scientists are still trying to understand what their actual contribution to the immune response might be, if any.
Indeed, these studies have been misinterpreted and used by some individuals to propagate unfounded claims regarding the level of immunity in the population, including Scott Atlas, a neuroradiologist and senior fellow at Stanford University’s Hoover Institution, according to this Buzzfeed News article. Another is ophthalmologist James Todaro, who claimed that these findings indicate that herd immunity could be achieved “once only 10-20% are infected with SARS-CoV-2”, which is much lower than most studies have estimated[9,10]. Todaro has also appeared in a viral video as part of America’s Frontline Doctors, a group that has spread false claims about the efficacy of hydroxychloroquine against COVID-19.
Shane Crotty, an immunologist and professor at the La Jolla Institute for Immunology, who co-authored the Cell and Science studies cited above, debunked these claims in the following Twitter thread:
1/ There are various tweets misinterpreting COVID-19 “pre-existing immunity” and making dangerous claims about herd immunity. Since many of those claims refer to our scientific papers, we will reiterate the facts. @SetteLab @ljiresearch @ScienceMagazine @CellCellPress pic.twitter.com/gCZwFMW1iU
— Prof. Shane Crotty (@profshanecrotty) August 12, 2020
“These are only speculations (no data) and because of their potential importance, it is key for scientists to test these ideas as quickly as possible. While scientists are racing as fast as possible, sophisticated research like this usually takes a lot of time and resources,” Crotty tweeted.
He also advised against relying on T cells for protection and neglecting to take other precautions. “T cells generally don’t completely prevent infections, they limit disease (make it shorter and/or less serious). Thus, wearing a mask is much more effective than hoping you and the people around you have pre-existing T cell memory. Wearing a mask stops infections,” he explained.
You can read the original National Geographic article here.
Scientists’ Feedback
The article accurately discusses the recent findings about the presence/relevance of T cell response against COVID-19. Indeed, both arms of adaptive immunity, humoral and cellular, contribute in different ways to the body’s fight against viral infections. What remains to be seen and explored in greater detail is how important the role of antigen-specific T cells is in protecting people from a re-infection or ameliorating the disease symptoms.
Also, to be able to comment on the role of protective antibodies against COVID-19, further studies are required to determine if, upon re-exposure to the virus, the immune system is able to generate effective titers of antibodies to neutralize the virus. The point raised by the article about the possible role of pre-existing immunity to other coronaviruses, such as those that cause the common cold, in the immunopathology of COVID-19 is also a very interesting concept which has to be studied more in detail to establish its relevance, if any.
One minor comment on the wording of the article: T cells do not always instruct the virus infected cells to self-destruct. Sometimes cytotoxic T cells are able to directly kill the infected cell as well.

Senior Research Fellow, A*STAR Infectious Diseases Labs
The article is very cautious about their statements and explains clearly what is known and what is suspected and therefore what needs to be clarified. SARS-CoV-2 is a very new virus that we still need to tame and the elicited immunity is not totally clear, because we don’t have enough perspective yet. More and more studies indicate that T cell immunity has a huge role in the fight against SARS-CoV-2 and the ongoing vaccine development has to keep this in mind. However, it does not mean that antibodies have no role at all and it is important to highlight the difference between what we observe in COVID-19 patients and how to develop a vaccine. It is possible that vaccination turns out to be very successful in eliciting very good antibodies, but only the future and more investigations can say.

Head of Training, Oxford University Clinical Research Unit
The article beautifully summarizes the results of recent studies which highlight the importance of the T cell response in immunity to the virus SARS-CoV-2. The immune response is a complex subject which is very difficult to describe in a lay manner, however, the author effectively utilized military metaphors to explain the basics of B and T cells in fighting disease. Most importantly, the key tenets of recent studies (particularly focusing on the publications of Grifoni et al. and Mateus et al.[1,2]) are communicated in a truthful manner using quotes from the authors of said studies. Other immunological experts also provided commentary on the recent finds. Importantly, the article is clear where the studies are published versus pre-review. The article refrains from overstating the importance of the findings, instead cautioning that the observed T cell responses may be of real relevance to vaccine development. However, we are as yet unsure whether these T cell responses translate into protection or reduction in disease severity.
REFERENCES
- 1 – Grifoni et al. (2020) Targets of T Cell Responses to SARS-CoV-2 Coronavirus in Humans with COVID-19 Disease and Unexposed Individuals. Cell.
- 2 – Mateus et al. (2020) Selective and cross-reactive SARS-CoV-2 T cell epitopes in unexposed humans. Science.
- 3 – Kumar et al (2020) Human T Cell Development, Localization, and Function throughout Life. Immunity.
- 4 – Sekine et al. (2020) Robust T cell immunity in convalescent individuals with asymptomatic or mild COVID-19. Cell.
- 5 – Le Bert et al. (2020) SARS-CoV-2-specific T cell immunity in cases of COVID-19 and SARS, and uninfected controls. Nature.
- 6 – Plotkin SA. (2020) Correlates of Protection Induced by Vaccination. Clinical and Vaccine Immunology.
- 7 – Long et al. (2020) Clinical and immunological assessment of asymptomatic SARS-CoV-2 infections. Nature Medicine.
- 8 – Ibarrondo et al. (2020) Rapid Decay of Anti–SARS-CoV-2 Antibodies in Persons with Mild Covid-19. New England Journal of Medicine.
- 9 – Britton et al. (2020) A mathematical model reveals the influence of population heterogeneity on herd immunity to SARS-CoV-2. Science.
- 10 – Randolph and Barreiro. (2020) Herd Immunity: Understanding COVID-19. Immunity.



