- Health
Scientific evidence shows that unvaccinated people are more likely to develop severe COVID-19 and die, contrary to claim in viral social media posts about Germany data
Key takeaway
Multiple scientific studies have shown that COVID-19 vaccines are highly effective at reducing the risk of severe COVID-19 and death. However, the COVID-19 vaccines aren’t 100% effective, so some vaccinated people will still become sick and die from COVID-19. In many countries in the world, there are far more vaccinated people than unvaccinated people. More vaccinated people being hospitalized is a reflection of the fact that vaccinated people far outnumber unvaccinated people, not that the vaccines work poorly.
Reviewed content

Verdict:
Claim:
More than 88% of ICU patients in Germany are vaccinated; the COVID-19 vaccines no longer protect against severe disease
Verdict detail
Misleading: The claim involved aggregating all vaccinated people into one group, without accounting for the fact that at-risk populations are overrepresented in the vaccinated population. This makes the hospitalization and mortality rate in the vaccinated group appear worse than the unvaccinated group (Simpson’s paradox). However, the higher risk of serious outcomes in this case is a reflection of the greater proportion of at-risk people in the vaccinated group, not the vaccines’ effectiveness.
Full Claim
“Vaccinated represent 88.4% of intensive care patients = so no protection against severe courses”; “In January 2022, 60% of Covid patients in intensive care units were unvaccinated, now 88.4% are vaccinated. [The Robert Koch Institute] and DIVI (all German intensive care units) report loss of protection against severe disease”
Review
Despite scientific evidence demonstrating that COVID-19 vaccination effectively reduces the risk of severe disease[1-5], claims that COVID-19 vaccines don’t work or even make things worse persist in online spaces and social media. Such claims, which were previously reviewed by Health Feedback, are commonly given a sheen of credibility through citations of official statistics as evidence.
A recent Twitter thread, published by a user named Olaf Garber on 6 November 2022, continued this trend. In the thread, Garber asked “Why are the unvaccinated disappearing from intensive care units?”
He claimed that data from the Robert Koch Institute (RKI) in Germany and the German Interdisciplinary Association for Intensive Care and Emergency Medicine (Deutschen Interdisziplinären Vereinigung für Intensiv- und Notfallmedizin; DIVI for short) “report loss of protection against severe disease”. He also claimed that the data showed “the vaccination no longer makes a difference”.
It’s not the first time that data from Germany was used to support such a claim. German fact-checking organizations Correctiv and the Deutsche Presse-Agentur investigated claims along the same lines independently. Both organizations found such claims to be misleading by omitting important caveats about the data.
Garber’s claim is no exception, as this review will explain below.
The base rate fallacy and imperfect vaccines
One of the problems with Garber’s claim is that it doesn’t account for the fact that the vast majority of people in Germany have been fully vaccinated. Our World in Data shows that to date, more than 76.2% of people in Germany have already completed the initial vaccination series (Figure 1).
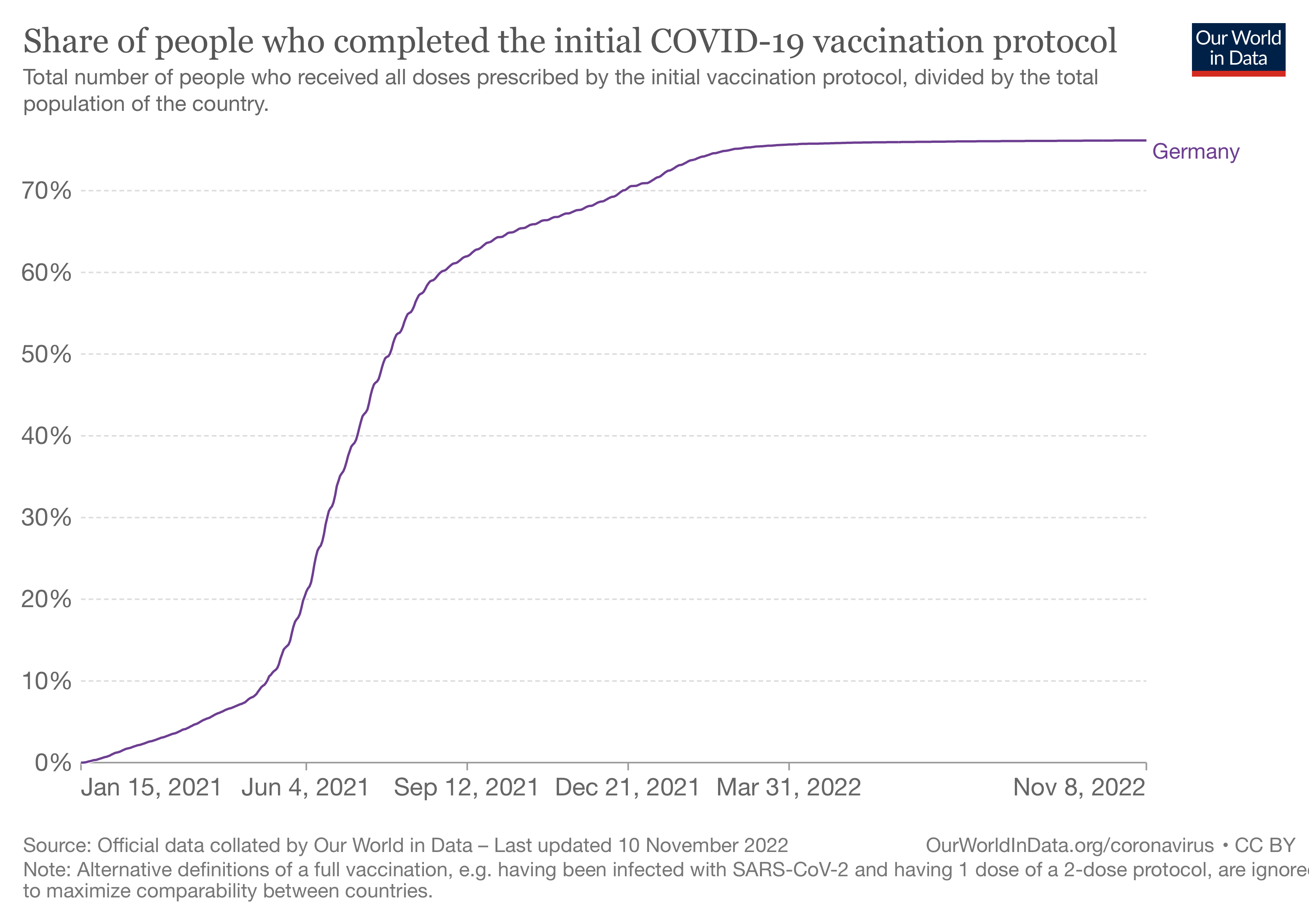
Figure 1. Proportion of people in Germany who are fully vaccinated (excludes boosters). Source: Our World in Data.
Studies showed that COVID-19 vaccines are highly effective against severe disease and death, and this remains the case even with the virus variants like Delta and Omicron. However, the COVID-19 vaccines aren’t 100% effective (no vaccine is), therefore among vaccinated people who do become infected (breakthrough infection), there will still be a small proportion who develop severe disease and some among them will die.
Because the majority of the German population have been vaccinated, the fact that vaccinated people make up the majority of ICU admissions isn’t unusual. By failing to recognize that the proportion of vaccinated people in hospitals primarily reflects the proportion of vaccinated people in the general population—rather than the vaccines’ effectiveness—Garber’s claim illustrates how the base rate fallacy works.

Figure 2. An example showing how the base rate fallacy works. Source: Science Up First.
Simpson’s paradox: the elderly are both more likely to be vaccinated and also more likely to die from COVID-19
Another factor to consider is that DIVI reported that the elderly make up the majority of COVID-19 ICU admissions. In fact, the graph in Garber’s third tweet in the thread, plotted using data from DIVI (downloaded here), showed this. Figure 3, taken from the DIVI website, also shows this.
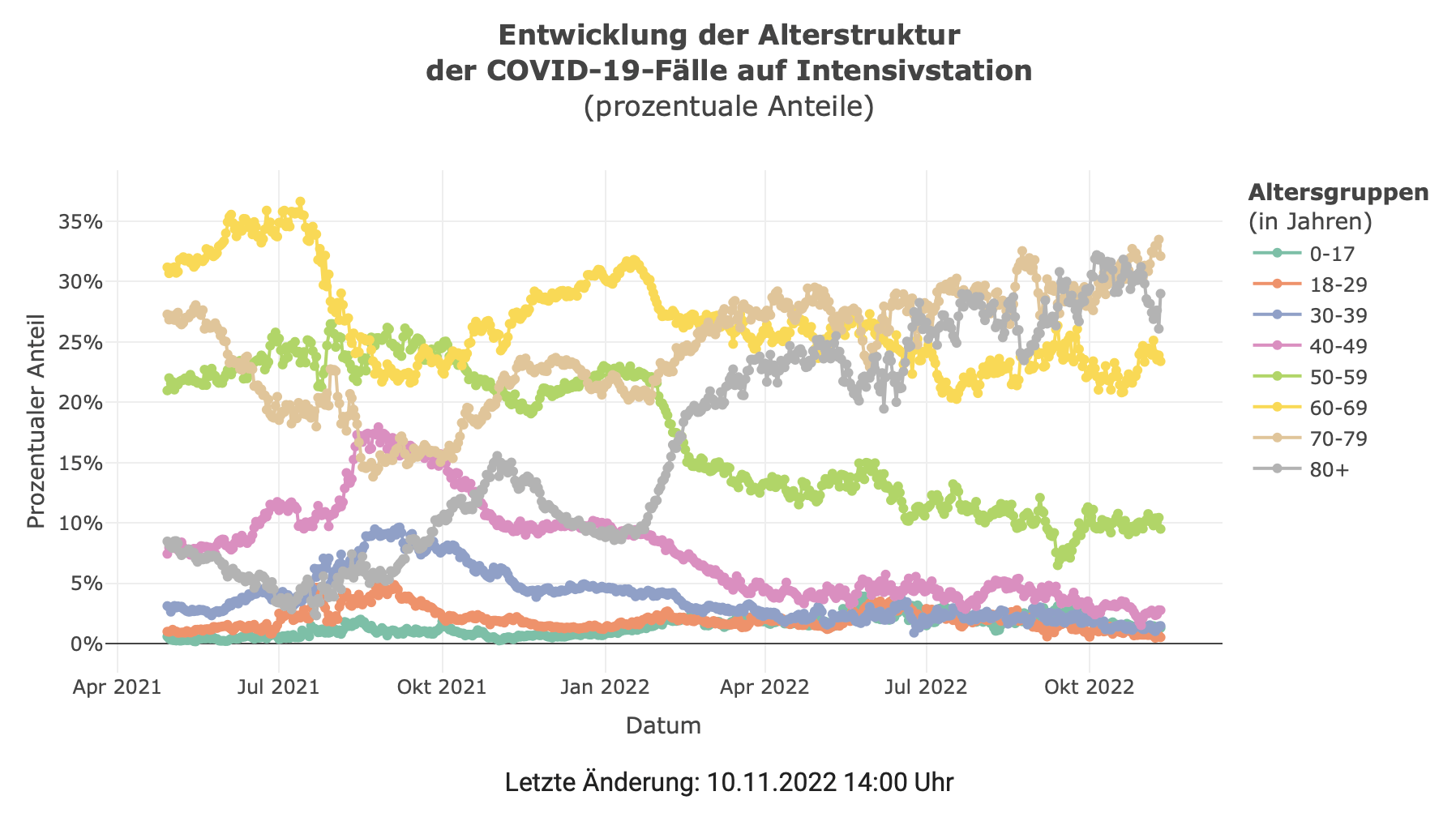
Figure 3. The proportion of COVID-19 patients in Germany’s ICUs, stratified by age group. Source: Robert Koch Institute. Data retrieved on 10 November 2022.
This is unsurprising. We already know that the elderly face the highest risk of hospitalization and death from COVID-19 (see Table 1 below).
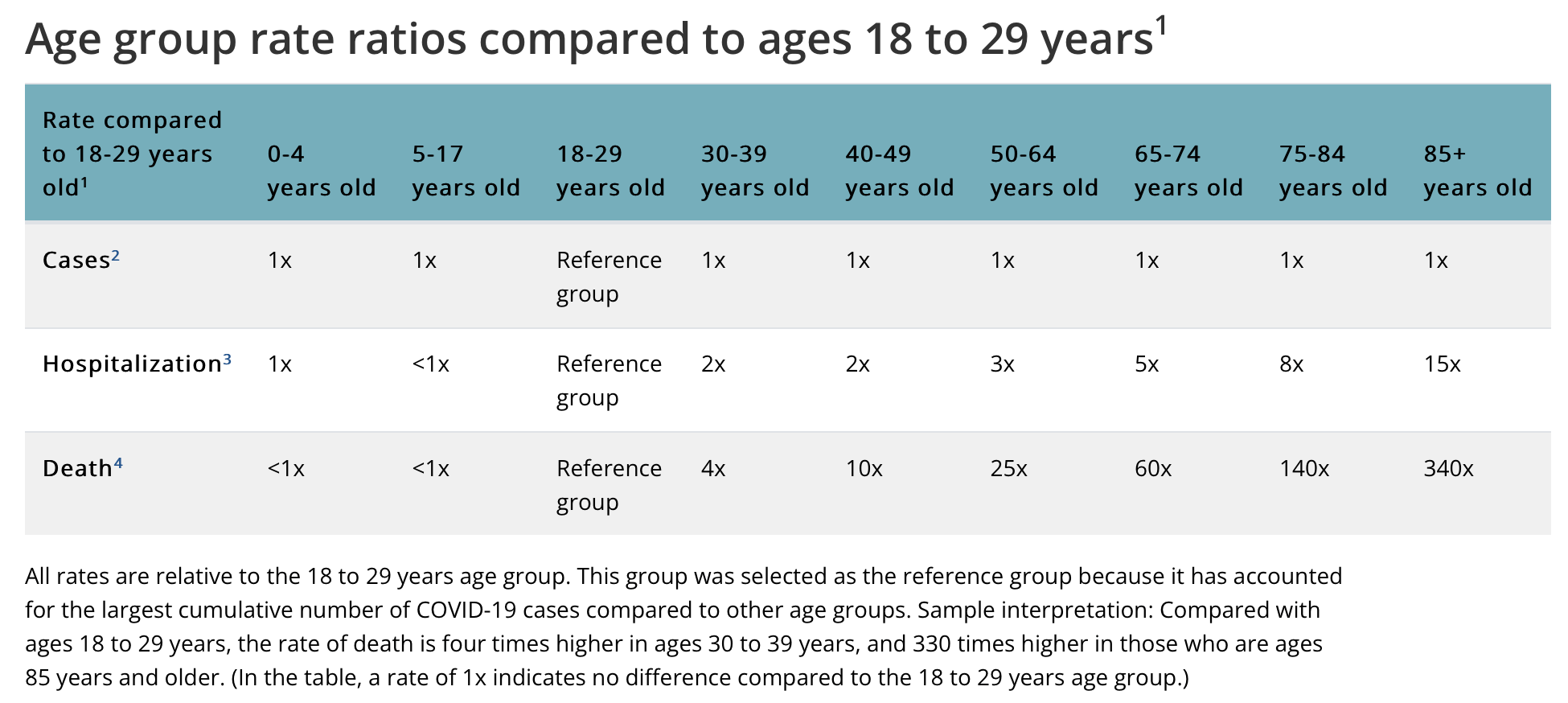
Table 1. The risk of disease, hospitalization, and death from COVID-19, relative to people aged 18 to 25. Source: U.S. Centers for Disease Control and Prevention.
On top of this, the elderly group also has the highest vaccine coverage compared to other groups (see Figure 4 below), at 90%.
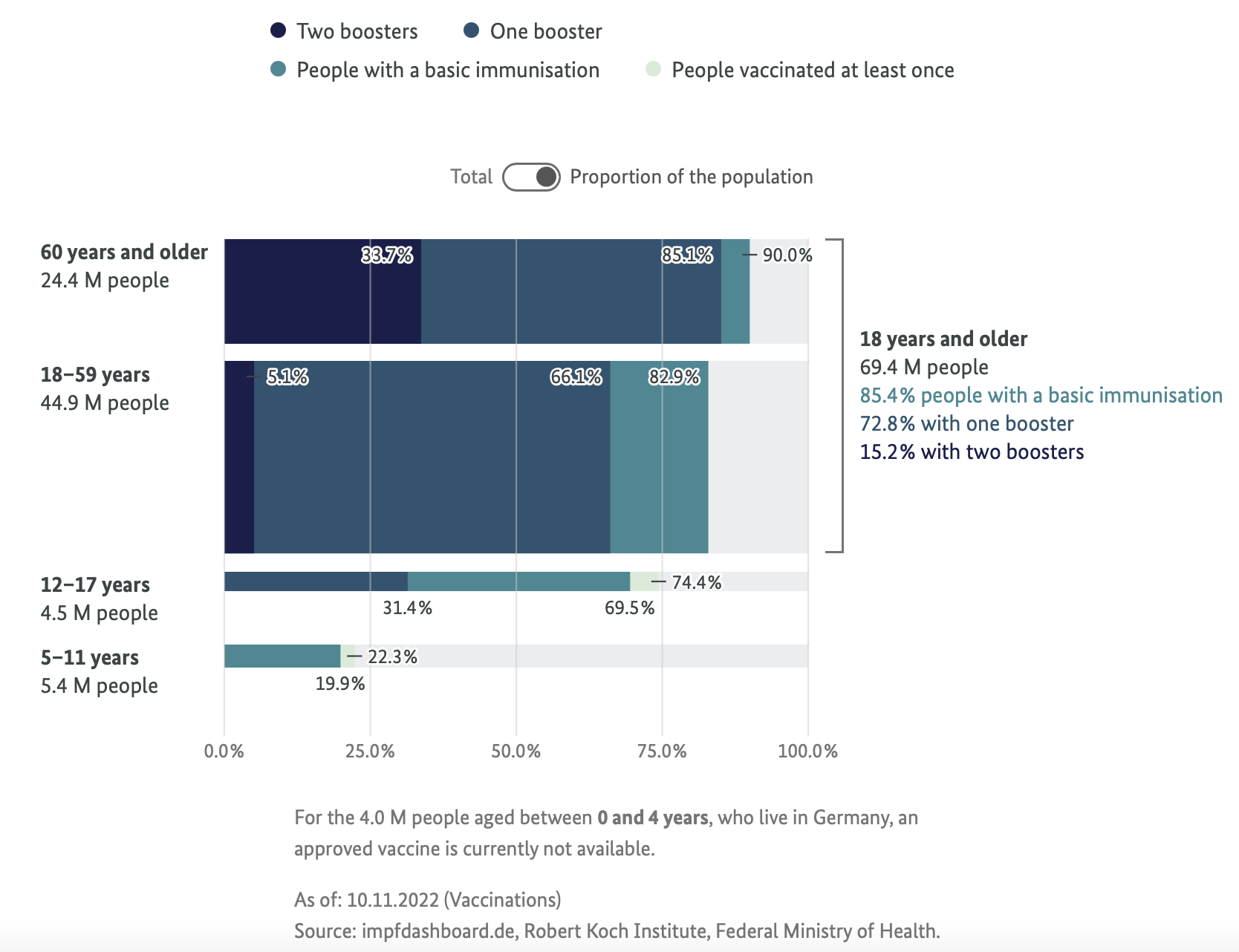
Figure 4. The proportion of vaccinated people in each age group in Germany. Source: Impfdashboard.de. Data retrieved on 10 November 2022.
However, Garber’s data comparing vaccinated and unvaccinated people didn’t break down the numbers based on age groups. By aggregating all vaccinated people together—without accounting for the fact that this group comprises more vulnerable people—it can make this group appear to be more likely to die, when the death rate is primarily due to the fact that the elderly are overrepresented in this group. This statistical artefact is known as Simpson’s paradox.
Overall, the proportion of vaccinated people among ICU admissions alone doesn’t allow us to form reliable conclusions about vaccine effectiveness, despite what Garber’s claim suggests.
Furthermore, the DIVI data used by Garber comes with another caveat: that the reason for ICU admission in people with COVID-19 is unknown. In a press release dated 6 October 2022, DIVI clarified that people counted among COVID-19 cases in the ICU were considered as such based on a positive SARS-CoV-2 test, but their admission to the ICU may have been for another reason: “cases are also listed […] that are being treated in intensive care due to another illness and for whom the Sars-CoV-2 diagnosis is not the focus of the disease or treatment”.
In such cases, the presence of these patients in the ICU doesn’t reflect on the vaccines’ effectiveness, since the reason they’re in the ICU isn’t because of COVID-19.
RKI reports show that unvaccinated people are more likely to be hospitalized and die from COVID-19
Monthly reports from the RKI actually do record COVID-19-specific outcomes (hospitalization, intensive care, death), categorized by age group and vaccination status.
The latest monthly report for October, released on 3 November 2022, showed that the proportion of unvaccinated people accounting for COVID-19 hospitalization, intensive care, and death was always greater than their proportion in the general population (Figure 5).
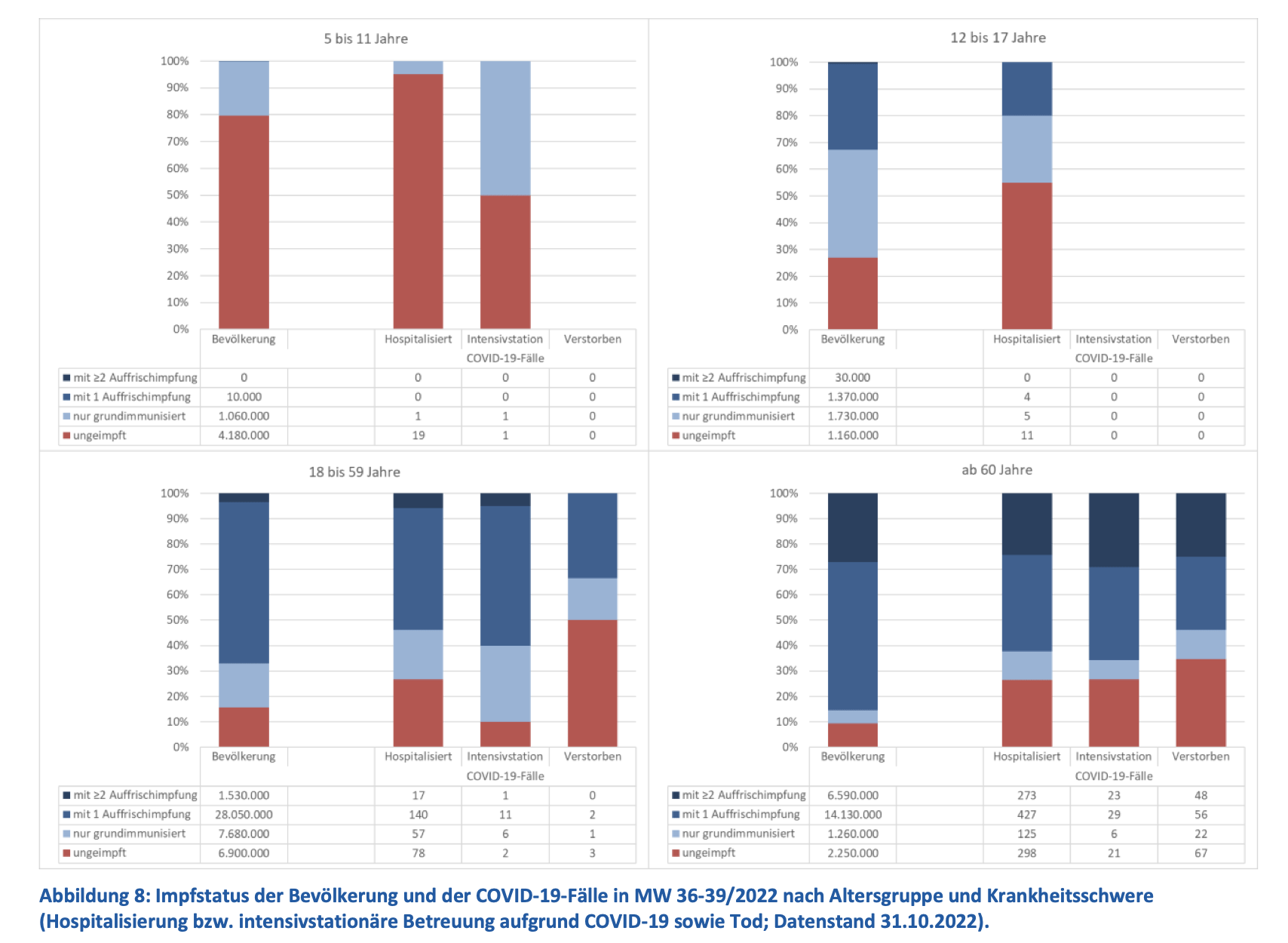
Figure 5. The proportion of unvaccinated (red) and vaccinated (all shades of blue) people who were hospitalized for COVID-19 (Hospitalisiert), admitted to intensive care (Intensivstation), or died (Verstorben), categorized by age group (5 to 11 years; 12 to 17 years; 18 to 59 years; 60 and above). The red portion of the bar for all three outcomes exceeds the red area in the general population (Bevölkerung) in nearly all cases except for those aged five to 11. Source: Robert Koch Institute. Data as of 31 October 2022.
In contrast, vaccinated people made up a smaller proportion of COVID-19 hospitalizations, intensive care admissions, and deaths relative to their numbers in the general population.
Figure 5 shows that when we account for the base rate of vaccinated people in the general population and difference in risk between age groups, we obtain a more accurate idea of how well the COVID-19 vaccines protect people from serious outcomes. The simplistic comparison made by Garber, in which vaccinated people are grouped together regardless of age group, obscures the fact that, all else being equal, vaccinated people are less likely to die of COVID-19 than unvaccinated people.
Conclusion
The problem with Garber’s claim isn’t because the figures used are incorrect; the figures were drawn from official sources. Where the problem lies is in the interpretation of these figures—caveats about the data, such as the different base rates of vaccinated and unvaccinated people and the uneven distribution of vulnerable people in the vaccinated and unvaccinated groups, distorted the true picture but were unaccounted for.
In contrast, when these caveats and limitations are addressed by researchers, the data shows that vaccinated people are less likely to develop severe COVID-19 and die compared to unvaccinated people.
REFERENCES
- 1 – Tenforde et al. (2021) Sustained Effectiveness of Pfizer-BioNTech and Moderna Vaccines Against COVID-19 Associated Hospitalizations Among Adults — United States, March–July 2021. Morbidity and Mortality Weekly Report.
- 2 – Andrews et al. (2022) Duration of Protection against Mild and Severe Disease by Covid-19 Vaccines. New England Journal of Medicine.
- 3 – Lauring et al. (2022) Clinical severity of, and effectiveness of mRNA vaccines against, covid-19 from omicron, delta, and alpha SARS-CoV-2 variants in the United States: prospective observational study. BMJ.
- 4 – Feikin et al. (2022) Duration of effectiveness of vaccines against SARS-CoV-2 infection and COVID-19 disease: results of a systematic review and meta-regression. Lancet.
- 5 – Stowe et al. (2022) Effectiveness of COVID-19 vaccines against Omicron and Delta hospitalisation, a test negative case-control study. Nature Communications.



