- Health
To date, no therapy has been proven effective for preventing or treating COVID-19, contrary to claim by Dolores Cahill
Key takeaway
Contrary to Cahill’s claims, no therapeutic strategy has been proven effective for preventing or treating COVID-19 as yet. Current evidence indicates that precautionary measures including frequent handwashing, cleaning and disinfection of frequently touched objects, use of masks, and social distancing are effective to help prevent the spread of COVID-19.
Reviewed content
Claim:
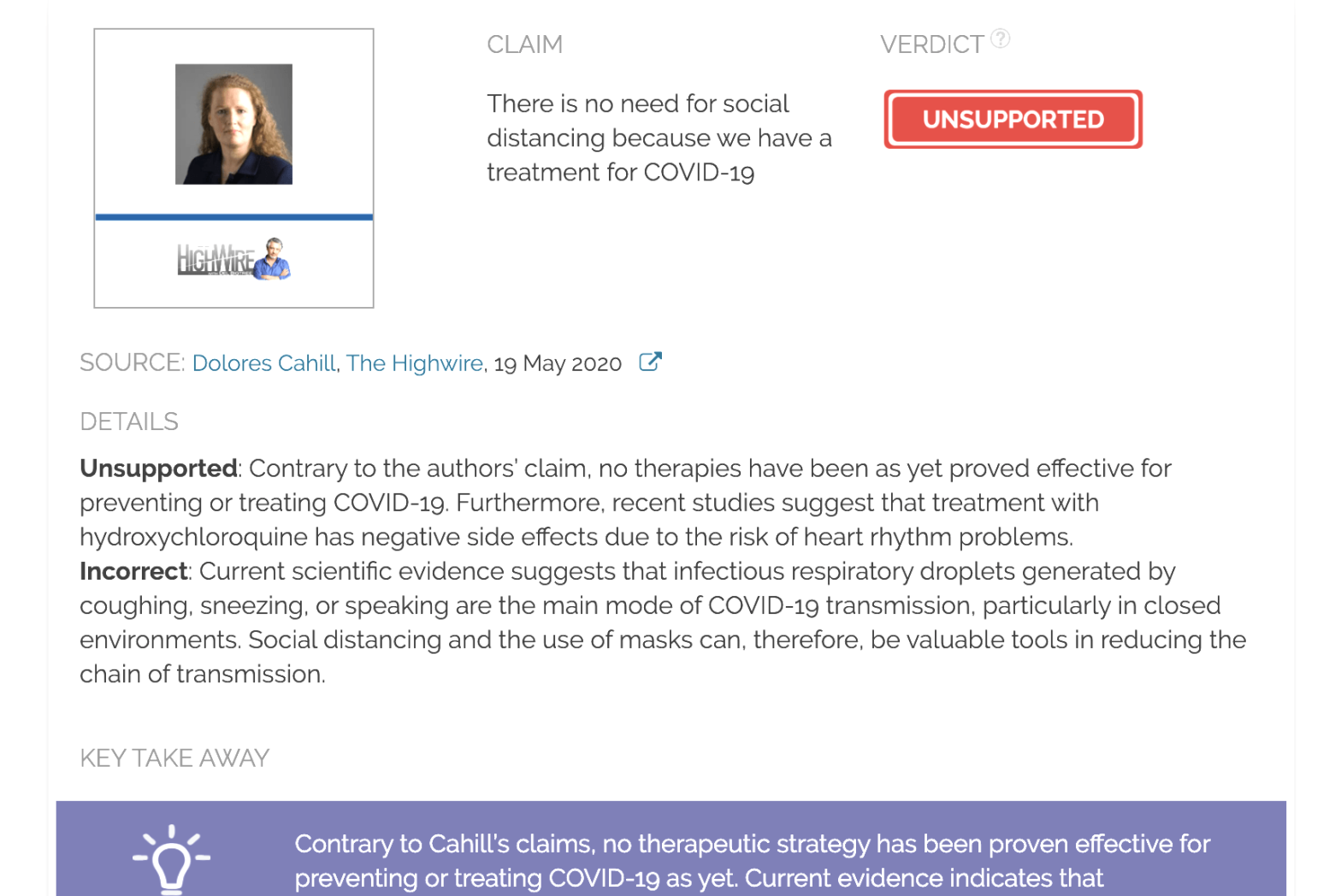
There is no need for social distancing because we have a treatment for COVID-19
Verdict detail
Unsupported: Contrary to the authors’ claim, no therapies have been as yet proved effective for preventing or treating COVID-19.
Incorrect: Current scientific evidence suggests that infectious respiratory droplets generated by coughing, sneezing, or speaking are the main mode of COVID-19 transmission, particularly in closed environments. Social distancing and the use of masks can, therefore, be valuable tools in reducing the chain of transmission.
Full Claim
“The reason why I think that this SARS-corona-2 should now be downed to safety class 1, which means you don’t require any social distancing, is because we now know we have a preventive strategy and we have a treatment”
Review
This video, published on 19 May 2020 on Facebook page The HighWire, features an interview between Del Bigtree and Dolores Cahill, a professor at University College Dublin who specializes in proteomics and the chairperson of the Irish Freedom Party. Cahill claims that “we have a preventive strategy and we have a treatment” for COVID-19, so “there is no need for social distancing, there is no need for masks.”
In the video, Cahill reiterates several claims she had made in an earlier interview on the YouTube channel Computing Forever, recently covered in this Health Feedback review. Specifically, Cahill’s claims that “nutrition, vitamins and hydroxychloroquine can prevent it [COVID-19] and treat it”. As Health Feedback explained, hydroxychloroquine has not been as yet proven effective to prevent or treat COVID-19 and the U.S. Food and Drug Administration (FDA) cautioned against its use without medical supervision due to risk of heart rhythm problems. At the moment, there is no drug that has been proven to be effective in treating or preventing COVID-19.
Vitamin and mineral supplementation are helpful in maintaining immune function, but the idea of consuming certain nutrients to “boost” the immune system and fight a COVID-19 infection can be misleading. Beneficial effects of supplementation are generally only observed when previous deficiencies were already present, as previously reviewed here and here.
Cahill also affirms that “once you have recovered from this virus, you are immune for life”, which is currently unsupported. We do know that immunity to other coronaviruses can be quite limited, but to determine how long COVID-19 immunity lasts will require more studies and a significant amount of time.
Cahill further states that “there is absolutely no need to be looking at models in these cases because we have such information and actual data around the world”. Models are limited by available data, and they have recently drawn criticism for inconsistencies and conflicting results. Yet, as summarized in a master question list from the U.S. Department of Homeland Security and contrary to Cahill’s claim, there is still a lot we do not know about COVID-19. The lack of epidemiological data is hindering the response to the pandemic and making experts rely on modeling to understand how the disease spreads and to evaluate the potential impact of control programs.
This Perspective article published in The New England Journal of Medicine highlights the challenges of modeling a new disease, however it also shows how disease models can help to make decisions and allocate resources towards disease control1, stating that “These models are a way to formalize what we know about viral transmission and explore possible futures of a system that involves nonlinear interactions, something that is almost impossible to do using intuition alone.” In this line, recent estimates from Columbia University researchers, published in a preprint, suggest that an early implementation of control measures may have led to substantially fewer cases and deaths in the U.S2.
Cahill uses these arguments, along with this table comparing SARS-CoV-2 and Ebola viruses, to assert that SARS-CoV-2 “should now be downed to safety class 1”. According to their relative risk, biological organisms are classified into four risk groups (RG), based on factors such as the mode of transmission of the microorganism and availability of preventive and treatment measures. Cahill correctly lists Ebola in RG 4, reserved for the most dangerous microorganisms. Although a comparison of RG between SARS-CoV-2 and Ebola is not explicitly stated, the table as presented may be misinterpreted to mean that SARS-CoV-2 and Ebola are currently in the same RG. However, the proposed classification of SARS-CoV-2, pending a definite risk assessment, is RG 3.
The table also contains inaccurate and incorrect data. First, it misleadingly conflates COVID-19 caused by the SARS-CoV-2 virus and the SARS pandemic outbreak from 2003, caused by the SARS-CoV-1 virus. Although both viruses belong to the same family, they are two different strains, as previously explained here. Phylogenetic analysis of coronaviruses also underscores this fact, showing that SARS-CoV-2 has a much stronger genetic similarity to a bat coronavirus isolated in the wild named RaTG13 (about 96% gene sequence identity)3 as compared to SARS-CoV-1 (about 79% gene sequence identity)4.
The table inaccurately states that Ebola, but not SARS-CoV-2, transmission occurs through the air. In fact, respiratory droplets have been identified as the main mode of COVID-19 transmission, as explained in this Health Feedback review. For this reason, the CDC recommends social distancing and cloth face coverings to reduce the spread of COVID-19, as previously explained.
In contrast, Ebola is not known to be an airborne virus. The World Health Organization states that “Airborne spread among humans implies inhalation of an infectious dose of virus from a suspended cloud of small dried droplets” and that “This mode of transmission has not been observed during extensive studies of the Ebola virus over several decades.” Rather, Ebola has been observed to spread by physical contact with infected body fluids, such as blood and vomit, or contaminated objects.
Also, it is an exaggeration to say that COVID-19 does not affect children. Children are indeed relatively less affected than adults, but pediatric cases of COVID-19, some of them severe, have been reported worldwide5. Recently, infection with COVID-19 in children has been associated with cases of multisystem inflammatory syndrome (MIS-C).
In summary, Cahill’s claim that there is no need for social distancing and masks is broadly based on inaccurate and incorrect data. One study, recently published in PNAS, showed that, in a closed environment, the small droplets of fluid emitted when a person speaks can remain suspended for tens of minutes6. Considering that high viral loads have been detected in saliva of both symptomatic and asymptomatic COVID-19 patients7, speech droplets arise as a very likely mode of COVID-19 transmission. Covering the mouth with a wet washcloth has been shown to dramatically reduce the number of droplets8 and proven effective in preventing transmission of other respiratory diseases9. Jeremy Howard, a research scientist at the University of San Francisco, and other scientists have also compiled a list of research publications supporting the use of face coverings for reducing disease transmission. All this evidence supports the use of masks and social distancing as valuable tools to reduce community transmission of COVID-19.
READ MORE
Other false claims regarding untested diagnostic methods, preventions, treatments, and cures for COVID-19 were previously addressed by Health Feedback here.
See a list of all coronavirus-related reviews written by Health Feedback here.
After the retraction of the study by Mehra et al. published in The Lancet, we removed it from this review and from the References list. The study, originally discussed in the first paragraph, claimed to show that COVID-19 patients treated with hydroxychloroquine had poorer survival and were more likely to experience abnormal heart rhythms.
REFERENCES
- 1 – Holmdahl et al. (2020) Wrong but Useful – What Covid-19 Epidemiologic Models Can and Cannot Tell Us. New England Journal of Medicine.
- 2 – Pei et al. (2020) Differential Effects of Intervention Timing on COVID-19 Spread in the United States. medRxiv.
- 3 – Zhou et al. (2020) A pneumonia outbreak associated with a new coronavirus of probable bat origin. Nature.
- 4 – Lu et al. (2020) Genomic characterisation and epidemiology of 2019 novel coronavirus: implications for virus origins and receptor binding. The Lancet.
- 5 – Sinha et al. (2020) COVID-19 infection in children. Lancet Respiratory Medicine.
- 6 – Stadnytskyi et al. (2020) The airborne lifetime of small speech droplets and their potential importance in SARS-CoV-2 transmission. PNAS.
- 7 – Zou et al. (2020) SARS-CoV-2 Viral Load in Upper Respiratory Specimens of Infected Patients. New England Journal of Medicine.
- 8 – Anfinrud et al. (2020) Visualizing Speech-Generated Oral Fluid Droplets With Laser Light Scattering. New England Journal of Medicine.
- 9 – Leung et al. (2020) Respiratory virus shedding in exhaled breath and efficacy of face masks. Nature Medicine.