- Health
Scientific evidence demonstrates that wearing face masks and implementing lockdowns reduce the spread of COVID-19
Key takeaway
Wearing face masks and implementing lockdowns are effective measures to reduce the spread of COVID-19. Face masks serve as physical barriers that reduce transmission of droplets that carry the virus from infected to uninfected people. Implementing lockdowns leads to significant reductions in physical interactions between people, which also reduces transmission of COVID-19.
Reviewed content
Verdict:
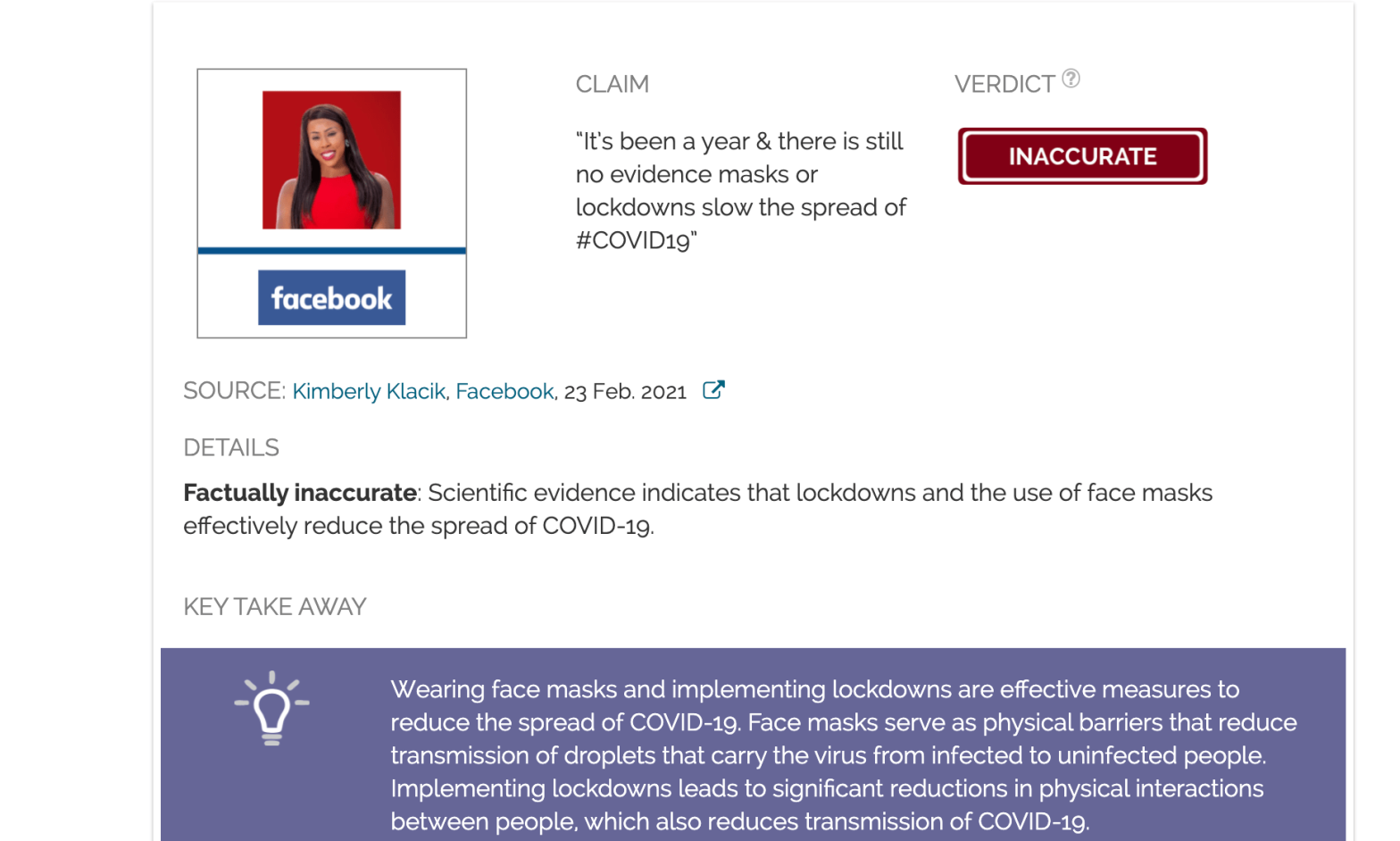
Claim:
“It’s been a year & there is still no evidence masks or lockdowns slow the spread of #COVID19”
Verdict detail
Factually inaccurate: Scientific evidence indicates that lockdowns and the use of face masks effectively reduce the spread of COVID-19.
Full Claim
“The fact that it’s been a year & there is still no evidence masks or lockdowns slow the spread of #COVID19, this has been a year long conspiracy theory that has devastated families from coast to coast.”
Review
On 23 February 2021, this Facebook post by Kimberly Klacik, a previous Republican nominee for Maryland’s 7th congressional district, claimed there is no evidence demonstrating that wearing face masks or implementing lockdowns reduce the spread of COVID-19. Over the past year, these public health measures have been used extensively around the world to reduce disease transmission. Several studies have analyzed the impact of these public health measures and concluded that they are effective at slowing the spread of COVID-19. While neither measure is 100% effective, they each reduce transmission of the disease significantly, as Health Feedback explained in earlier reviews.
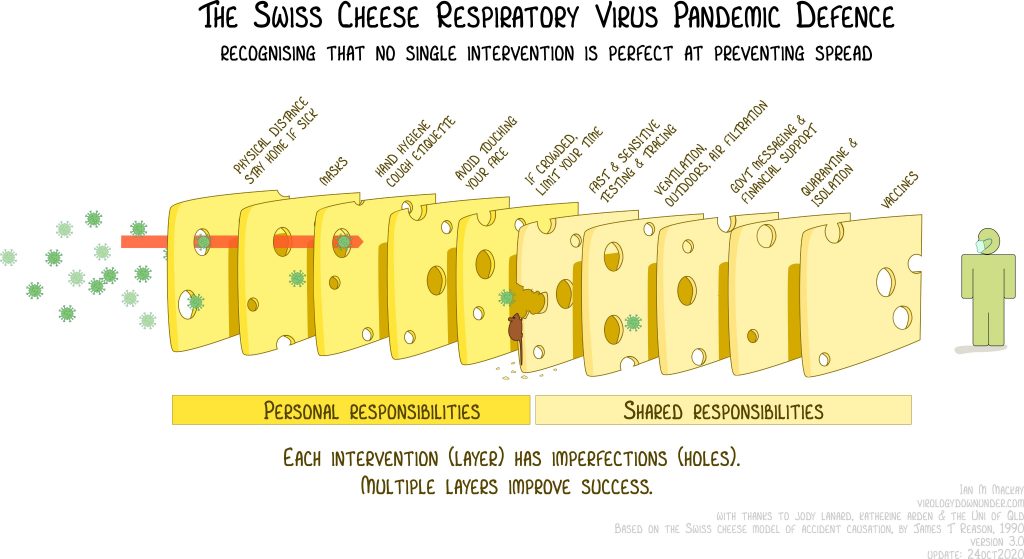
Combining multiple, imperfect measures provides the greatest protection against the spread of COVID-19, as this graphic by virologist Ian Mackay illustrates simplistically:
Evidence shows that wearing face masks reduces the spread of COVID-19
The virus that causes COVID-19, SARS-CoV-2, is transmitted, in part, by small respiratory droplets, which can be released into the air by infected people. Face masks reduce the spread of these respiratory droplets by serving as physical barriers. This reduces the risk of droplets breathed out by an infected person being inhaled by uninfected people nearby.
Frontline healthcare workers use medical-grade N95 respirators, as many are exposed to high levels of the virus while treating COVID-19 patients. During the early stages of the COVID-19 pandemic, it was unclear whether nonmedical masks were effective in reducing disease transmission. The WHO initially advised against widespread mask-wearing by the public, citing the risk of a false sense of security and a mask procurement burden for healthcare workers, as did the U.S. Centers for Disease Control and Protection (CDC).
When scientific evidence demonstrated that the virus was primarily spread through respiratory droplets, the WHO recommended that the general public wear face masks on June 5, 2020. Since June 2020, the use of face masks to reduce the spread of COVId-19 has been mandated in many countries and most U.S. states. The WHO provided more detailed advice on mask use in December 2020, recommending that people age 12 or older always wear face masks in public indoors areas without adequate ventilation, even when following physical distancing measures.
With the rapid onset of the COVID-19 pandemic, it was difficult and potentially unethical to carry out randomized controlled trials to test the effectiveness of wearing face masks to reduce the spread of the disease[1]. However, the gradual adoption of wearing face masks provided an opportunity to study their effectiveness using observational data.
Noah Haber, a meta-science researcher, wrote in November 2020:
“On masks and mask mandates, there may never be a direct, reliable, and actionable study of their population-level benefits. What we have instead is a collection of evidentiary bits and pieces; and when these are taken all together they say that masks are certainly somewhat effective—maybe even very effective—at slowing the spread of SARS-CoV-2.”
A study published in May 2020 provided what the authors describe as the first evidence that wearing face masks reduced the spread of COVID-19 between family members[2]. Among hundreds of people in Beijing, the use of face masks by infected people and their family contacts before the onset of symptoms reduced disease transmission by 79%.
A study published in February 2021 comparing different states in the U.S. showed that early introduction of statewide mask requirements reduced COVID-19 case numbers by 1% per day compared with states that did not adopt these measures[3]. By 31 October 2020, the mask mandates led to a 58% lower risk of COVID-19 in these early-adopter states. The authors of the study stated, “Our findings support statewide mask requirements to mitigate COVID-19 transmission”.
A group of international researchers reviewed the evidence regarding the effectiveness of wearing face masks on reducing COVID-19 transmission, and recommended that governments implement mask use requirements[1]. In the review, the researchers highlighted the following points in favor of their recommendation:
“Nonmedical masks use materials that obstruct particles of the necessary size; people are most infectious in the initial period postinfection, where it is common to have few or no symptoms; nonmedical masks have been effective in reducing transmission of respiratory viruses; and places and time periods where mask usage is required or widespread have shown substantially lower community transmission.”
Well-fitting masks and widespread use of face masks increase their effectiveness in reducing disease transmission. Tests carried out by the CDC using lab dummies found that wearing a cloth or surgical face masks reduced the number of droplets released into the air after a cough by approximately 50%[4]. Furthermore, when a cloth mask is worn over a surgical mask, this is increased to 85% protection. Exposure to infected respiratory droplets was reduced by 96.4%, when the person coughing and a nearby person were each wearing cloth and surgical masks.
As described in a review published in the Annals of Internal Medicine in December 2020[5]:
“Growing evidence that SARS-CoV-2 is airborne indicates that infection control interventions must go beyond contact and droplet measures (such as handwashing and cleaning surfaces) and attend to masking and ventilation. Observational evidence suggests that masks work mainly by source control (preventing infected persons from transmitting the virus to others), but laboratory studies of mask filtration properties suggest that they could also provide some protection to wearers (protective effect). Even small reductions in individual transmission could lead to substantial reductions in population spread.”
Although evidence from large-scale clinical trials isn’t available, there is ample observational evidence that wearing face masks reduces the spread of COVID-19.
Lockdowns also reduce the spread of COVID-19
Lockdowns have been implemented in many countries since the beginning of the pandemic to reduce COVID-19 transmission. By reducing the movements of members of the public, this approach aims to reduce contact between infected and uninfected people and therefore reduce the risk of transmission. Since then, many scientific studies concluded that lockdowns are highly effective at reducing the spread of the disease.
For example, an analysis of the lockdown measures in Wuhan, which included stopping all public transport and banning motor vehicle use, showed that before the lockdown, each COVID-19 case led to four other infections. Following the lockdown, this fell to almost one, effectively halting the growth in new infections[6].
The effectiveness of this public health measure led several European countries to introduce lockdowns as COVID-19 spread quickly in the following months. A study that looked at the effects of different interventions across 11 European countries found that lockdowns reduced disease transmission by 81%[7].
In the U.S., a study contrasting states with and without stay-at-home orders found that they had a significant impact on the spread of COVID-19[8]. Among the 45 states that introduced stay-at-home orders, COVID-19cases doubled every two to six days before the measures were implemented. After the stay-at-home orders, the rise in new cases slowed significantly, and the doubling rate of cases increased to nine to 70 days. By contrast, the states without stay-at-home orders had much less improvement in slowing the rate of new COVID-19 cases.
Some countries reduced the spread of COVID-19 without implementing lockdown measures, although this coincided with changes in public behaviour, including physical distancing.
Lockdowns are often temporary public health measures that are used when the infection rate of a disease is not adequately controlled. The WHO’s published advice states that lockdowns “can slow COVID‑19 transmission by limiting contact between people”. However, they recognize the potential negative impact of a lockdown and insists that other measures are implemented to control the spread of the disease once the lockdown ends:
“WHO recognizes that at certain points, some countries have had no choice but to issue stay-at-home orders and other measures, to buy time.“
But they also emphasized that:
“Governments must make the most of the extra time granted by ‘lockdown’ measures by doing all they can to build their capacities to detect, isolate, test and care for all cases; trace and quarantine all contacts; engage, empower and enable populations to drive the societal response and more.”
Conclusion
The claim by Kimberly Klacik that there is no evidence for the effectiveness of face masks or lockdowns in reducing COVID-19 spread is inaccurate. As these public health measures have been implemented over time around the world, scientists have been able to analyse their impact on the spread of COVID-19. Face masks help to reduce the transmission of respiratory droplets, which are a major route of disease spread. Lockdowns or stay-at-home orders reduce contacts between infected and uninfected people and several studies showed that these measures slowed the spread of COVID-19.
REFERENCES
- 1 – Howard et al. (2020) An evidence review of face masks against COVID-19. Proceedings of the National Academy of Sciences.
- 2 – Wang et al. (2020) Reduction of secondary transmission of SARS-CoV-2 in households by face mask use, disinfection and social distancing: a cohort study in Beijing, China BMJ Global Health.
- 3 – Rebeiro et al. (2021) The impact of state mask-wearing requirements on the growth of covid-19 cases in the United States. Clinical Infectious Diseases.
- 4 – Brooks et al. (2021) Maximizing Fit for Cloth and Medical Procedure Masks to Improve Performance and Reduce SARS-CoV-2 Transmission and Exposure, Morbidity and Mortality Weekly Report
- 5 – Czypionka et al. (2020) Masks and Face Coverings for the Lay Public. Annals of Internal Medicine.
- 6 – Pan et al. (2020) Association of Public Health Interventions With the Epidemiology of the COVID-19 Outbreak in Wuhan, China. Journal of the American Medical Association.
- 7 – Flaxman et al. (2020) Estimating the effects of non-pharmaceutical interventions on COVID-19 in Europe. Nature
- 8 – Lurie et al. (2021) Coronavirus Disease 2019 Epidemic Doubling Time in the United States Before and During Stay-at-Home Restrictions. The Journal of Infectious Diseases.